SEBASTIAN LOCATION (New Location!)
13852 US Hwy 1
Sebastian, FL 32958
VERO BEACH LOCATION
- AminoFix injection for Plantar Fasciitis & Achilles Tendonitis
- Arch Pain
- Bunions And Bursitis
- Certified Wound Care Specialist
- Comprehensive Foot And Ankle Surgery
- Congenital Foot And Ankle Deformities
- Corns And Calluses
- Diabetic Foot Care
- Flat Feet
- Foot And Ankle Fractures
- Fungal Skin Infections
- Hammertoes
- Laser treatment for fungal nails
- Heel Spurs
- Metatarsal Disorders
- Pediatric Foot And Ankle Problems & Injuries
- Plantar Fasciitis
- Plantar Warts
- Reconstructive Surgery Of The Foot And Ankle
- Sports Related Injuries
- Traumatic Surgery Of The Foot And Ankle
- Treatment Of Charcot Foot And Ankle Deformities
- Treatment Of Ingrown, Fungal And Thickened Nail Conditions
Welcome to the Patient Information Center! Here you will find information about the most common foot and ankle ailments. Click on any of the issues below to find out more about specific problems and what treatment options are available. Here you will also find links to interesting websites pertaining to podiatry. If you have any questions, feel free to Contact Us through the website or give us a call!
Common Ailments
- Achilles Tendon Disorders
- Acute Inflammation
- Ankle Fracture
- Ankle Sprain
- Bunions
- Cavus Foot
- Charcot Foot
- Chronic Ankle Instability
- Crossover Toe
- Diabetic Complications and Amputation Prevention
- Diabetic Foot Care Guidelines
- Diabetic Peripheral Neuropathy
- Equinus
- Flexible Flatfoot
- Fractures of the Fifth Metatarsal
- Ganglion Cyst
- Gout
- Haglund’s Deformity (pump bump)
- Hallux Rigidus
- Hammertoes
- Heel Pain
- Ingrown Toenail
- Lisfranc Injuries
- Malignant Melanoma of the Foot
- Morton’s Neuroma
- Osteoarthritis of the Foot and Ankle
- Pediatric Flatfoot
- Pediatric Heel Pain
- Peroneal Tendon Injuries
- Plantar Fasciitis (Heel Pain)
- Plantar Wart (Verruca Plantaris)
- Posterior Tibial
- Puncture Wounds
- Rheumatoid Arthritis in the Foot and Ankle
- Sesamoid Injuries in the Foot
- Tailor’s Bunion
- Tarsal Coalition
- Tarsal Tunnel Syndrome
- Toe and Metatarsal Fractures
Helpful Information & Links
The path to board certification by the American Board of Podiatric Surgery (ABPS) begins after graduating from an approved podiatric surgical residency program after which our doctors pass a rigorous written examination to become board qualified. Next, doctors spent up to 6 years of their initial practice time collecting various patient cases which demonstrate to the ABPS their decision-making, competency, and skills as a foot and ankle surgeon. After submission of these cases, detailed review, and acceptance to the ABPS, doctors sit for the ABPS oral examination held in Chicago, IL.
- Dr. Paradoa has satisfied requirements by the ABPS to become board certified in Foot, Reconstructive Rearfoot/Ankle Surgery.
Our patients can feel confident that they are being treated by a foot
and ankle surgeon who has dedicated years of her education, training,
and experience to achieving board certification status by the American
Board of Podiatric Surgery.
The American Board of Podiatric Surgery website
has a wealth of information about podiatry and the requirements that
must be met.
A Doctor of Podiatric Medicine (DPM) is to the foot and ankle what a dentist is to the mouth, or an ophthalmologist to the eye — a doctor specializing in the prevention, diagnosis and treatment of foot disorders resulting from injury or disease. A DPM makes independent judgments, prescribes medications and performs surgery. The human foot has a complex interrelation with the rest of the body which means that it may be the first area to show signs of serious conditions such as diabetes and cardiovascular disease. Since the podiatric physician is often the first to detect symptoms of these disorders, he or she becomes a vital and sometimes lifesaving link in the health care team.
The American College of Foot & Ankle Surgeons is a professional society of thousands of foot and ankle surgeons. Their website contains a plethora of information about advances in podiatry and connects its members to share that knowledge.
FootHealthFacts.org is the official consumer website of the American College of Foot and Ankle Surgeons. This is a wonderful resource of information! From what foot injuries Olympians have suffered from during the 2012 London Olympics to a growing trend in lawn mower accidents, you will find interesting, informative and compelling articles in the world of Podiatry.
Patient Forms
Please print and fill out these forms so we can expedite your first visit:
In order to view or print these forms you will need Adobe Acrobat Reader
installed. Click here to download it: 
- Home >
- Articles >
- Bone/Joint/Tendon >
- Ankle >
- Tarsal Coalition
What is a Tarsal Coalition?
A tarsal coalition is an abnormal connection that develops between two bones in the back of the foot (the tarsal bones). This abnormal connection, which can be composed of bone, cartilage, or fibrous tissue, may lead to limited motion and pain in one or both feet.
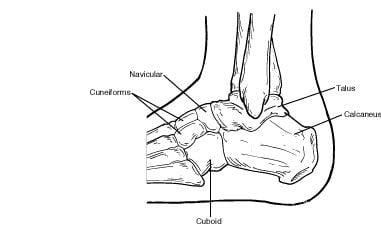 The tarsal bones include the calcaneus (heel bone), talus, navicular, cuboid, and cuneiform bones. These bones work together to provide the motion necessary for normal foot function.
The tarsal bones include the calcaneus (heel bone), talus, navicular, cuboid, and cuneiform bones. These bones work together to provide the motion necessary for normal foot function.
Causes
Most often, tarsal coalition occurs during fetal development, resulting in the individual bones not forming properly. Less common causes of tarsal coalition include infection, arthritis, or a previous injury to the area.
Symptoms
While many people who have a tarsal coalition are born with this condition, the symptoms generally do not appear until the bones begin to mature, usually around ages 9 to16. Sometimes there are no symptoms during childhood. However, pain and symptoms may develop later in life.
The symptoms of tarsal coalition may include one or more of the following:
- Pain (mild to severe) when walking or standing
- Tired or fatigued legs
- Muscle spasms in the leg, causing the foot to turn outward when walking
- Flatfoot (in one or both feet)
- Walking with a limp
- Stiffness of the foot and ankle
Diagnosis
A tarsal coalition is difficult to identify until a child’s bones begin to mature. It is sometimes not discovered until adulthood. Diagnosis includes obtaining information about the duration and development of the symptoms as well as a thorough examination of the foot and ankle. The findings of this examination will differ according to the severity and location of the coalition.
In addition to examining the foot, the surgeon will order x-rays. Advanced imaging studies may also be required to fully evaluate the condition.
Non-surgical Treatment
The goal of non-surgical treatment of tarsal coalition is to relieve the symptoms and reduce the motion at the affected joint. One or more of the following options may be used, depending on the severity of the condition and the response to treatment:
- Oral medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be helpful in reducing the pain and inflammation.
- Physical therapy. Physical therapy may include massage, range-of-motion exercises, and ultrasound therapy.
- Steroid injections. An injection of cortisone into the affected joint reduces the inflammation and pain. Sometimes more than one injection is necessary.
- Orthotic devices. Custom orthotic devices can be beneficial in distributing weight away from the joint, limiting motion at the joint and relieving pain.
- Immobilization. Sometimes the foot is immobilized to give the affected area a rest. The foot is placed in a cast or cast boot, and crutches are used to avoid placing weight on the foot.
- Injection of an anesthetic agent. Injection of an anesthetic into the leg may be used to relax spasms and is often performed prior to immobilization.
When is Surgery Needed?
If the patient's symptoms are not adequately relieved with nonsurgical treatment, surgery is an option. The foot and ankle surgeon will determine the best surgical approach based the patient's age, condition, arthritic changes, and activity level.
Appointment Request
Our Locations
Find us on the map
Hours of Operation
Our Regular Schedule
Vero Beach Location
Monday:
9:00 AM-5:00 PM
Tuesday:
9:00 AM-5:00 PM
Wednesday:
9:00 AM-5:00 PM
Thursday:
9:00 AM-5:00 PM
Friday:
9:00 AM-12:00 PM
Saturday:
Closed
Sunday:
Closed
Sebastian Location
Monday:
9:00 AM-5:00 PM
Tuesday:
9:00 AM-5:00 PM
Wednesday:
9:00 AM-5:00 PM
Thursday:
9:00 AM-5:00 PM
Friday:
9:00 AM-12:00 PM
Saturday:
Closed
Sunday:
Closed
